 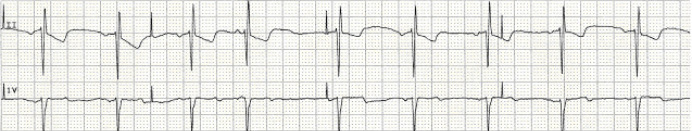
May exhibit features of atrial pacing, ventricular pacing or both.the major terminal portion of the QRS complex is located on the opposite side of the baseline from the ST segment and T wave. ST segments and T waves should be discordant with the QRS complex i.e.Left epicardial pacing lead placement results in a QRS morphology similar to RBBB.Right ventricle pacing lead placement results in a QRS morphology similar to LBBB.Morphology of p wave dependent of lead placement but may appear normal.Epicardially placed leads result in smaller pacing spikes than endocardially placed leads.Bipolar leads result in a much smaller pacing spike than unipolar leads.Amplitude depends on position and type of lead.Vertical spikes of short duration, usually 2 ms.The appearance of the ECG in a paced patient is dependent on the pacing mode used, placement of pacing leads, device pacing thresholds, and the presence of native electrical activity. Paced ECG – Electrocardiographic Features ACC/AHA/HRS 2008 Guidelines for Device-Based Therapy of Cardiac Rhythm Abnormalities.The 2002 American College of Cardiology, American Heart Association and North American Society for Pacing and Electrophysiology guidelines for implantation of cardiac pacemakers.Note this differs from magnet application to an Implantable Cardioversion Defibrillator (ICD) which results in defibrillator deactivation.In asynchronous ventricle pacing there is a risk of pacemaker-induced ventricular tachycardia.Asynchronous modes deliver constant rate paced stimuli regardless of native rate of rhythm.Usually initiates an asynchronous pacing mode – AOO, VOO, or DOO.This mode varies with pacemaker set-up and manufacturer.Applying a magnet to a pacemaker will initiate the magnet mode.Atrial channel function is suspend during a fixed periods following atrial and ventricular activity to prevent sensing ventricular activity or retrograde p waves as native atrial activity.Ventricular pacing occurs if no native ventricle activity for set time following atrial activity.Atrial pacing occurs if no native atrial activity for set time.atrial fibrillation or flutter.ĭDD – pacing and sensing the atria and ventricles Used in patients with chronic atrial impairment e.g.Similar to AAI mode but involving ventricles instead of the atrium.Used in sinus node dysfunction with intact AV conduction.If no native activity sensed for pre-determined time then atrial pacing initiated.If native atrial activity sensed then pacing is inhibited.Superseded by the NASPE/BPEG Defibrillator Code. Refers to presences of anti-tachydysrhythmia functions.Reflects the programming options available for pacemaker set-up or presence of rate modulation ability.  
Position IV: Programmability / Rate Modulation.more than one pacing site within the atria or biatrial pacing Allows indication of multiple stimulation sites within one anatomical area e.g.Sensors may measure and respond to variables including vibration, respiration, or acid-base status. Indicates ability for rate modulation designed to altered heart appropriately to meet physiological needs e.g.I = Sensed activity results in inhibition of pacing activity.T = Sensed activity results in triggering of paced activity.Refers to pacemakers response to sensed native cardiac activity.Refers to the location where the pacemaker senses native cardiac electrical activity.The code is expressed as a series of up to five letters.The NASPE/BPEG Generic (NBG) Pacemaker Code was last revised in 2002, although many textbooks still use the previous version from 1987.Classification follows pacemaker code developed by the North American Society of Pacing and Electrophysiology (NASPE) and the British Pacing and Electrophysiology Group (BPEG).Pacemakers are classified by the nature of their pacing mode. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
